Team X-Ray Standards Review
Laura S. Harkin, DMD
I’m the owner of a third-generation dental practice. My father was a special person who cared for his patients as much as he did his dentistry. One important piece of advice that he gave was to make sure that my patient records were always complete and pristine. He said, “Anything that you are sending to the laboratory or to a specialist, even down to how you write your lab script or note, must be precise. And the reason is not only to minimize adjustment at the end but to also set an expectation for the same level of care returned by the lab or specialist.”
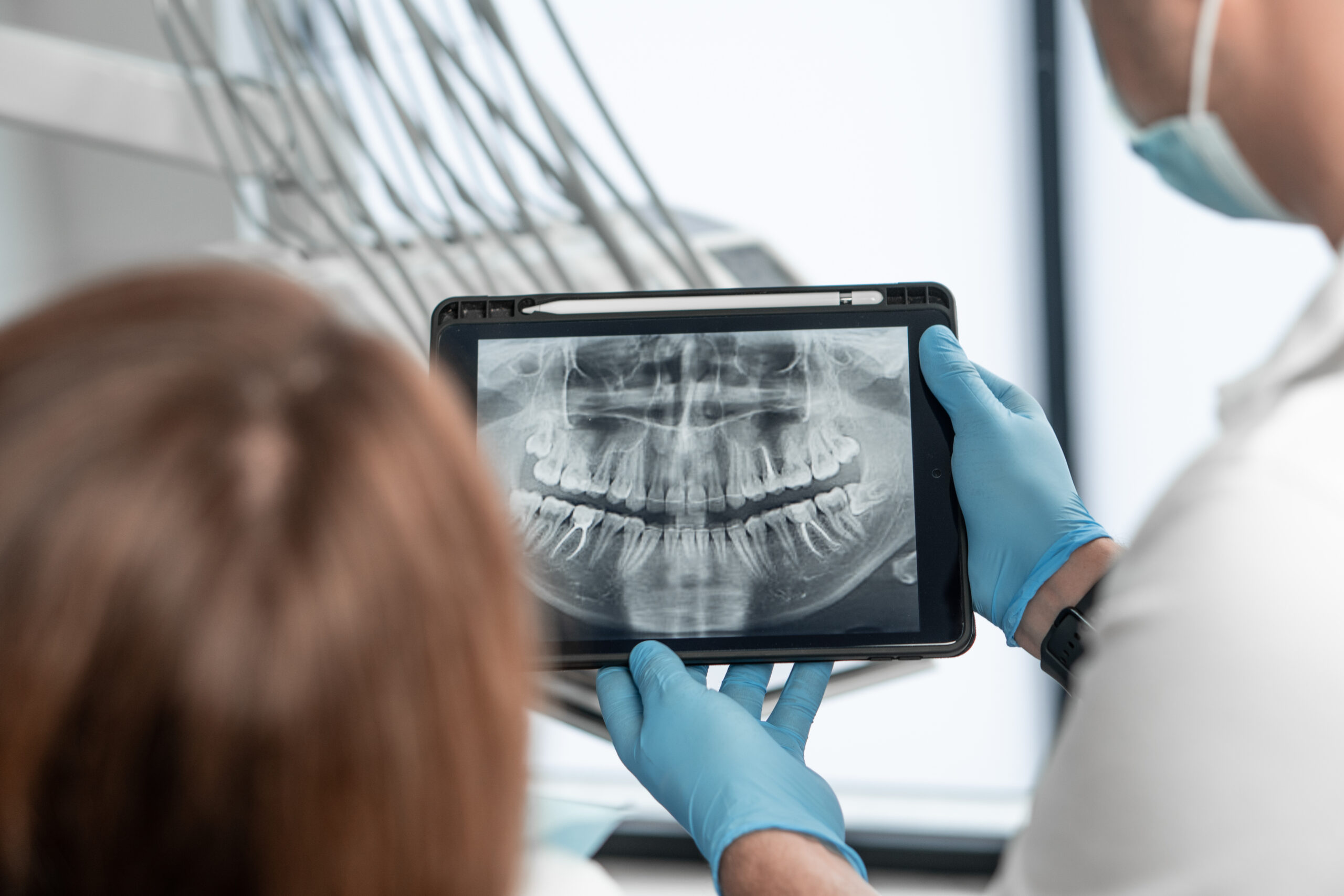
As a team, we have spent time evaluating our models and photos to discuss how they can be improved and to recognize our highest standard. Recently, I became a little concerned about some of the radiographs we’d taken in the office. I encountered a few bitewings in which I was able to see the bone levels or the image wasn’t anterior enough to check the distal of the canine. So, as a team, we set aside time to review current x-rays and discuss the diagnostic qualities that we seek to achieve in each type.
A team huddle provides built-in time and a safe place to do something like this. While reviewing the images, it became very clear that the team knew how to take vertical and horizontal bitewings. They also had a clear visual for how the images should look. Sometimes, however, a team member was shy about retaking an x-ray for they worried that a patient would be uncomfortable with the process. Other times, I imagine, they felt pressed for time and hurried to move down their checklist.
Our review of images reinforced the level of care we collectively aim to achieve in all facets of our clinical day. Just as we strive for beautiful, mounted study casts, we take our x-rays with intention for our ourselves, our referral sources, and, above all, our patients. Consider taking a team meeting to share each other’s tips and tricks for taking x-rays in patients with difficult anatomy, a gag reflex, or missing teeth. Our own team members have a wealth of knowledge that sometimes doesn’t move from one treatment room to the next!
Related Course
The Intentional Hygiene Exam
DATE: September 5 2024 @ 8:00 pm - September 5 2024 @ 9:00 pmLocation: Online
CE HOURS: 1
Date: September 5, 2024 Time: 8 – 9 pm ET Speakers: Michael Rogers DDS & David Gordon DDS Description: Is your hygiene program an interruption to your day? Or is…
Learn More>